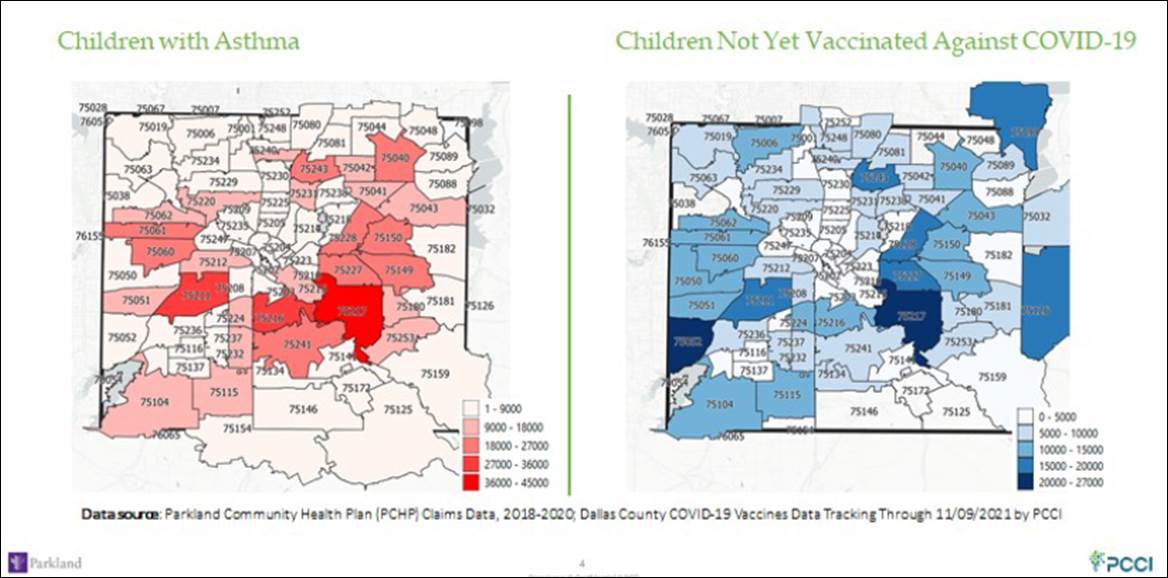
The areas of Dallas with the highest risk for COVID-19 infection are also the areas least protected against the virus, according to new data from the Parkland Center for Clinical Innovation. It shows the ZIP codes with the lowest COVID-19 vaccination rates are also the areas with the highest levels of asthma, a comorbidity that can increase the severity of the virus in children.
Vaccines are now available for kids ages 5 to 11, but for several reasons, many low-income neighborhoods still lag behind others when it comes to their vaccination rates. Risk factors like heart disease, cancer, and obesity have made the virus much more deadly for adults. And while the virus has been less lethal for children, asthma increases the likelihood of a more severe infection in pediatric cases.
Part of the solution will be outreach. Internet access and healthcare providers are often limited in these neighborhoods. In ZIP codes 75217, 75211, 75228, 75227, and 75243, overlapping high pediatric asthma and low COVID-19 pediatric vaccination rates collide. Pleasant Grove’s 75217 has the region’s highest pediatric asthma rate and the lowest COVID-19 pediatric vaccination rate in Dallas County. Cockrell Hill and Oak Cliff’s 75211 has the same problem. These are two of Dallas’ poorest areas and have already been ravaged by the pandemic. The other ZIP codes include Far East Dallas and Mesquite (75228), southeast Dallas (75227), and northeast Dallas around Forest Lane (75243).
According to the American Lung Association, 11 percent of families below the poverty line ($26,500 for a family of four) had children with asthma in 2018. Only 6.8 percent of families who made at least $52,400—200 percent of the poverty line—had children with asthma. A study from the National Institutes of Health also found that substandard housing and environmental triggers are linked to greater asthma morbidity and mortality for low-income and Black and Latino children living in urban areas.
Dallas is making progress on youth vaccinations: more than 50 percent of high school students and more than one in three middle school students have been vaccinated. The issue is that many unvaccinated children are likely to have asthma.
The original strain of COVID-19 didn’t impact children as severely. But after the rise of the more contagious delta variant, children went from representing 4 percent of cases early in the pandemic to 25 percent of all cases in recent weeks. Schools opening, the relaxation of public health measures, reduced mask-wearing and social distancing, and a lack of vaccine for children was all part of the increase in pediatric cases.
In 19 months since the beginning of the pandemic, around 6.4 million children have been diagnosed with COVID-19 (about 8.5 cases per 100 children). In Texas, 211,000 cases have been reported among public school students within the first three months of the school year. According to PCCI, around 25,000 children around the country have been hospitalized, and 600 children have died from COVID-19 complications. For the 2018-2019 flu season, there were 366 flu deaths nationwide and 39,000 hospitalizations, which means that the COVID-19 death toll is 64 percent higher than a typical flu season.
Children with comorbidities like asthma are particularly vulnerable to severe COVID-19 infections, hospitalizations, and death, but we have a solution to protect at-risk children.
“The vaccine elicits a strong, protective immune response and is over 90 percent effective against COVID-19 infections, hospitalizations, and deaths,” writes Dr. Yolande Pengetnze, PCCI’s vice president of clinical leadership. “With this new tool in our arsenal, we are one step closer to winning the battle against COVID-19. Vaccines, however, only work if they are administered to people who need it.”






