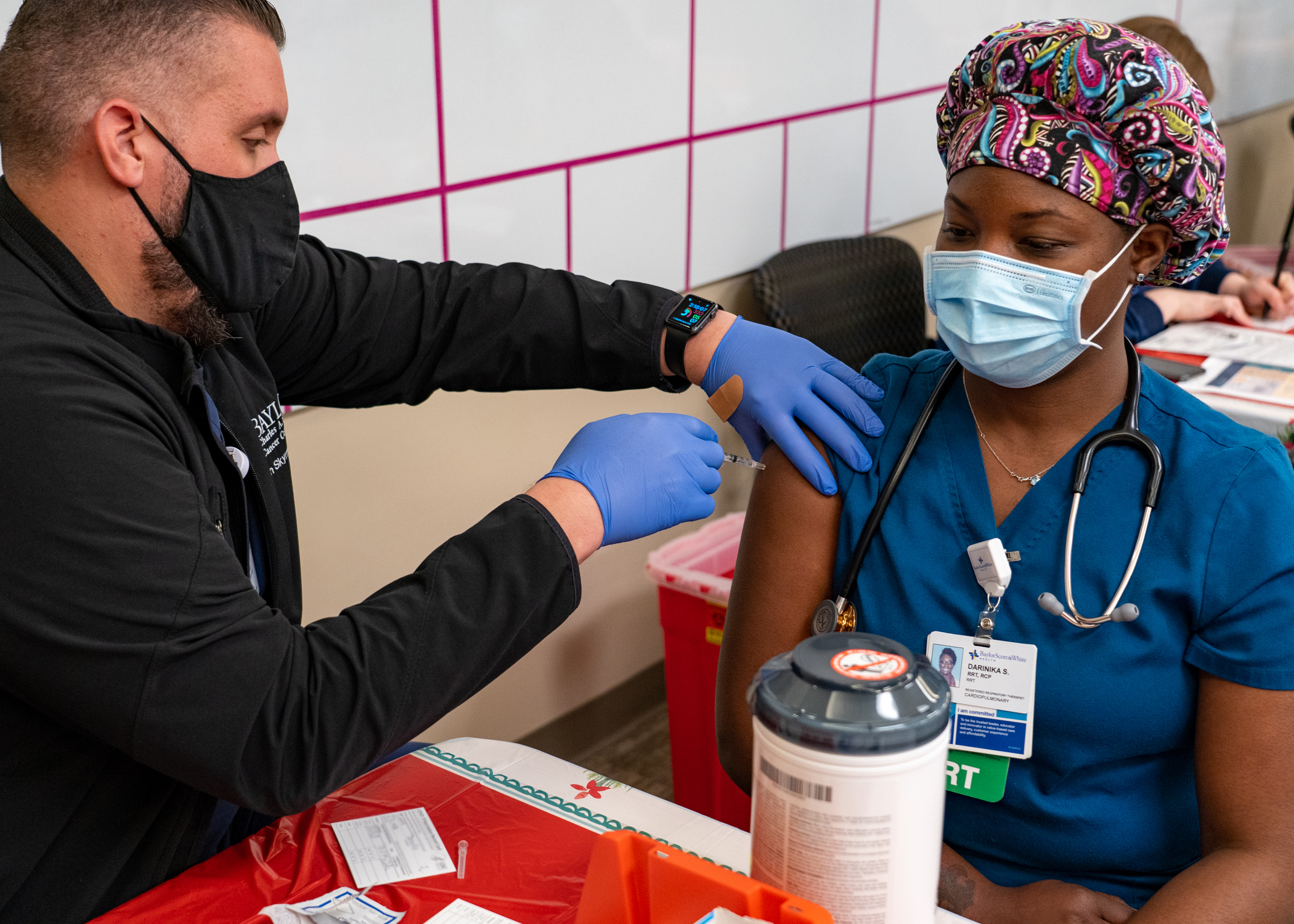
News reports are full of breathless accounts of UPS delivering COVID-19 vaccines, celebratory vaccinations, and major relief from healthcare workers about the beginning of the end of the pandemic. Still, the real work was done months ago, as health systems created protocols for efficient and effective vaccine distribution to its employees.
Hospitals had to make arrangements with limited and changing information. Pharmaceutical companies, the FDA, federal, state, and local governments all influenced the timing, amount, and manner in which the vaccines were distributed. At Baylor Scott & White Health, a multi-disciplinary team of physicians, nurses, pharmacists, human resources staffers, and legal leadership built a playbook for distributing the vaccine. Clear and aligned communication was essential to ensure the vaccine was correctly distributed throughout Texas’s most extensive nonprofit health system, which reaches from near the Oklahoma border to Austin.
Additional vaccines are complicating the process. The Pfizer version requires ultra-cold storage and two injections three weeks apart. The Moderna iteration includes two shots four weeks apart. The soon-to-arrive Johnson & Johnson vaccine will be just one shot. Health systems will be forced to create unique protocols for each one to maximize the number of vaccinations they can give their employees in the weeks ahead.
But even as they create protocols and workflows, health systems still do not have clarity about who is eligible for the vaccine, how many vaccines they are getting, or any last-minute instructions from the manufacturers about its application. “We couldn’t put the dot on every I and cross every T until we got the final drug regulations for Pfizer,” says Janice Walker, the Executive Vice President and Chief Nursing Officer for Baylor Scott and White Health. “We had the framework, and then we had to back up and ensure that at the very last hour, everything was covered.”
The state is the arbiter of who is eligible and how many vaccines each facility is receiving. However, it is acting off of federal guidance and applications that providers submitted to receive the doses. The state department of health has released guidance for two tiers of healthcare workers who will be eligible. Tier one includes hospital staff, home health workers, senior living staff, and residents. The second tier allows outpatient healthcare workers who see COVID-19 patients, community pharmacy staff, freestanding emergency room staff, school nurses, community health workers, and mortuary and death services staff to receive the vaccine.
But beyond those tiers, hospitals and providers are pretty much in the dark about who will be next. With emotions running high, it is essential that decisions about high-priority populations are well-explained and logical. This responsibility will be left up to the hospital, though they will just be following state orders. Leaders have to frame the process in a way that will be palatable to those who may have to wait to be vaccinated, especially those who are at greater risk than the general public. Others will have lifestyle pressures they’ll want addressed. “Everybody is going to the game, event, or celebration,” says Tammy Cohen, vice president of pharmacy services for BSW. “You may be coming in different doors, you may be getting very different times, but we’re all going to get to the vaccine.”
The vaccine will be distributed to healthcare employees over the coming weeks, but the public will have to wait a bit longer. The CDC has already released tiers of the general public beyond healthcare. First responders, police, manufacturers of the vaccine, pregnant women, and toddlers are next in line, followed by military personnel, critical infrastructure workers, and children. The federal guidelines are not binding, and it will be up to each state to interpret those rules and implement their own system, and the health providers will follow suit. Most states are sticking pretty close to the CDC’s recommendations.
Though this may be the beginning of the end, it will be months before life can safely resume to anything we might consider normal. Walker put it well: “The vaccine is the glimmer of hope and the light at the end of the tunnel for the world. But we know that that tunnel is still extremely long.” Patience, everyone.