To work inside a county hospital like Parkland, you have to keep a steady gait while the ground shifts beneath your feet. That’s what Katie Mapula loves about her job as the nursing director over all five intensive care units and burn center operations. You think you know what the day will look like, and then—boom—there’s an urgent rush to make order of fresh chaos.
On the morning of September 29, 2021, Mapula was making order of yet another exhausting COVID surge. The swath the Delta variant cut through Dallas had filled every bed in the ICU and then some. She had already converted 12 more beds on the Medical Surgery floor to handle the growing demand when—boom—a startling notification rang in.
A firefighter called mayday on the channel that reaches the entire city emergency system. There had been an explosion in South Dallas. Ten were on the way. That meant Mapula needed 10 rooms. She had negative space available, but the injured were 20 minutes out. She had some time.
Mapula initiated a call to the medical directors to see which ICU patients might be stable enough to be downgraded. She checked in with Emergency for updates, trying to anticipate the need for ICU versus acute care in the burn unit. After someone sent her a news photo from the scene—half of a two-story building collapsed and charred—she knew she needed rooms in the ICU. As word of the mass casualty event made its way up to leadership, the chief clinical officer sent a page to every doctor in the organization. People moved fast. Mapula got on the line with Bed Access Management and then Environmental Services to disinfect the freed rooms.
“One thing I did realize through this whole thing is that you really do have to engage everyone,” Mapula says. “The Environmental Service person who’s cleaning the room is just as important as the doctor who tried to get the patient out.”
When the first survivor was wheeled up from Trauma, the room was still drying.
One firefighter and four civilians had suffered minor injuries, so the call for 10 turned out to be three firefighters, all critically injured with second- and third-degree burns. The first to arrive in the burn unit was rookie officer Pauline Perez. Oak Cliff born and raised, Perez took a lot of bull from the guys at Station 25 for wearing eyelash extensions—“Are those fans on your eyes?” they’d tease—but shift by shift she was proving her worth.
After Perez, they brought in Ron Hall, a veteran firefighter of 40 years. Hall’s last day (a delayed retirement, much to his wife’s chagrin) was scheduled for January, a little more than three months away.
It would take a few more days for Captain Christopher Gadomski to join his colleagues in the burn unit. Just as the surgeon was getting ready to save his ravaged legs, Gadomski coded and had to be resuscitated. In his 28 years fighting fires, he had gotten banged up, sure, but he had never spent even a night in a hospital. Still, the physical pain was only part of the agony.
Hall would be with the other firefighters in the waiting room if it wasn’t for Gadomski. After Gadomski made captain and left their Pleasant Grove station for a newer facility in Oak Cliff, Hall moved to dispatch. A few months from retirement, Hall picked up the phone and there was Gadomski saying his station needed an experienced driver engineer. Hall cussed and hung up. Gadomski called him back. “You’re going to retire a dispatcher,” he said. “You’re not even a firefighter anymore.” On Hall’s first day in Oak Cliff, his wife, Mona, drove up to Station 25 to give Captain Gadomski a piece of her mind. Gadomski swore up and down he’d take care of her husband.
“That was the worst feeling in the world,” Gadomski says, remembering the moment he saw Mona through the hospital room window. “I was scared to death of seeing her more than anything. Anything.”
But Mona knew: there was no way the captain could have seen this coming.
Just hours before the firefighters ended up in Mapula’s care, they had been responding to a call about a carbon monoxide leak at an apartment complex in South Dallas. When Perez stepped inside the affected unit, she heard a hiss and saw the oven’s shattered glass—hit by a bullet a man had intended for his pregnant girlfriend, they’d later learn. Perez had just turned to evacuate when she was pitched off her feet, engulfed in flames. The blast pushed Ron Hall against a door frame, the strongest part of the building, causing his joints to take the brunt of the impact and rip apart like the seams of an old t-shirt.
Looking back, Gadomski wonders if he might have died in the blast, or maybe why he didn’t. For a moment, time stopped and he was floating. Then it felt as if someone picked him up and set him down. In reality, the force sent him smashing from the breezeway through at least two walls into another apartment. He tried to lift himself up when he heard Hall screaming—and then looked down to see his own tibia bones. His pants were shredded, and his phone was lost somewhere in the rubble. But somehow his radio was still in his back pocket.
The first responder to Gadomski’s mayday call pulled up to find Perez looking like a scarecrow, skin hanging from her arms. She had sheetrock embedded in her flesh from clawing and crawling out of the wreckage. Hall, suffering burns that left him unrecognizable, also managed to pull himself out and walk away on a broken leg.
When he was pulled from the burning building, Gadomski was cognizant enough to correct a well-meaning rescuer who suggested that the ambulance head to the nearest hospital.
“No, you idiot, I’m burned!” Gadomski shouted. “Take me to Parkland!”
Parkland is one of 74 burn programs in the nation verified by the American Burn Association, and it’s the only verified burn unit for pediatrics and adults in North Texas. The Burn Center offers advanced treatments, such as hydrotherapy tank beds, though services impact patients beyond Parkland’s walls. The hospital offers a free course to train EMS professionals on how to begin interventions on burn patients before they pull into the ER. There’s also a survivor network and support services for children and adults, including a child life specialist who helps pediatric burn patients take the often stressful step of returning to school. A burn-survivor summer camp gives kids the opportunity to ride horses and swim without feeling self-conscious in their own (often new) skin. “Our tentacles go out quite a bit,” says Katie Mapula. Maintaining Parkland’s burn verification status is one of her many responsibilities.
Mapula has spent her entire career, more than 13 years, inside Parkland, ever since she landed a residency straight out of the University of Virginia nursing program. She got her first glimpses of the hospital as a teenager watching the TLC docuseries Trauma: Life in the E.R. An adrenaline junkie, she dreamed of working as a flight nurse but decided to get experience in the ICU and ER first. Yet after having kids (she delivered at Parkland, naturally), the prospect of a risky career on a helicopter gave her pause. Instead, Mapula took a left turn into leadership. She now works with 15 nurse leaders who oversee about 350 nurses throughout the ICU and burn center, covering nearly 100 beds in total.
The role suits her. “She probably has the most vivacious personality of anyone that I have ever met,” says Chaplain Elaine Maddox of Dallas Fire-Rescue, who is now all too familiar with the Parkland waiting room. “She’s always trying to keep the tempo upbeat, to be a facilitator to the families and to come alongside the patients.”
“Katie was just awesome as far as being a communicator, being compassionate and a doer,” says Patty Armstrong, Gadomski’s mother and a retired nurse. “She did not let the grass grow under her feet for one minute.”
No surprise, Mapula was a cheerleader her whole life, up through college. “That nature is just in me,” she says. “I have an eternal optimism.” That energy propels her through long hours, and at home she makes an effort give her little girls a window into her professional life. This past Christmas, Mapula’s daughters made cards for every one of her patients. “I want them to see the hard work and grit and resilience,” she says. “That all this stuff really does pay off.”
Freeing up beds wasn’t Mapula’s only challenge the day of the explosion. Those movie scenes depicting crowds of first responders, filling hospital lobbies elbow-to-elbow as a show of support for ailing colleagues? They are no exaggeration. Hundreds of emergency personnel from Dallas and other cities, every fire chief in the area, the police chief, and the mayor, too, all pulled into the Parkland parking lot. There were at least 50 people crowding the waiting room at any given time. But Mapula knew better than to keep the firefighters away from their brethren.
“One thing I learned about the firefighter community is they absolutely need that level of support,” she says. “They’re used to being together at the station. It’s a brotherhood, and so they need each other to get through all that’s happening medically.”
Mapula arranged to keep Hall, Perez, and Gadomski in adjacent rooms. While a rotating four-man crew of firefighters kept a 24-hour watch in the corridor, she did her best to manage the flow of visitors. But she soon realized that first responders were often swinging through the burn unit undetected after dropping new patients at the ER. “They found ways to have more visitors than I’m sure I even know,” Mapula says. “They’re hilarious, right? They kept us laughing the whole time.”
Kathy Doherty, Parkland’s interim vice president of surgical services, notes Mapula’s ability to treat individual patients with compassion while also protecting the hospital as a whole in the midst of a pandemic. “It’s a delicate balance between supporting the firefighters, their families, and their extended family in the fire department but also supporting the organization,” she says. “As far as having to limit visitors, ensure everyone was wearing face masks, that there weren’t too many big groups gathering together, and making sure that some patients weren’t getting special care versus others—you always want to be mindful of that. And Katie does that exceptionally well. She’s able to look at the big picture.”
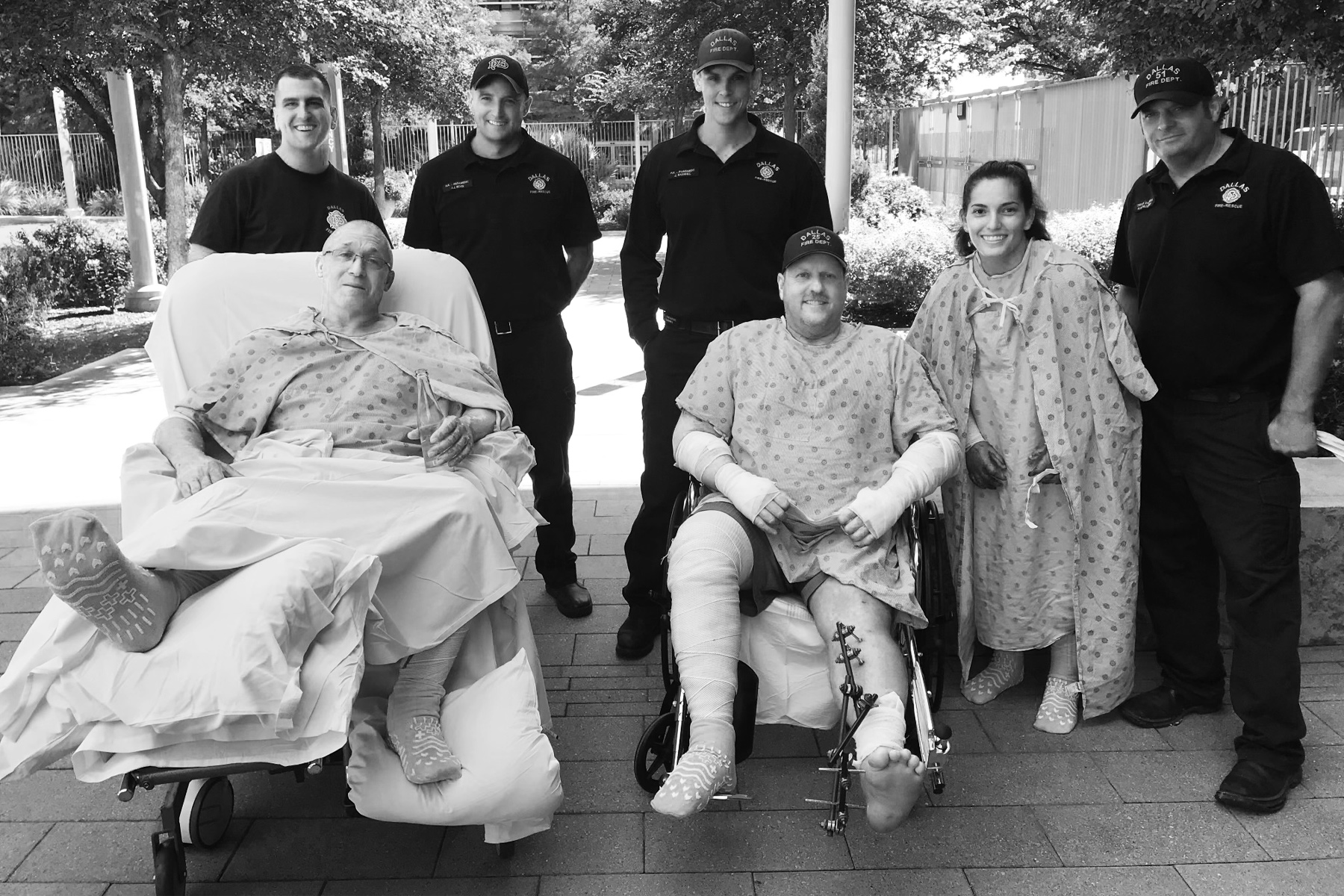
Thirteen days after the accident, when Captain Gadomski’s condition was stable, Mapula rallied a team of six nurses to give the firefighters some fresh air. Taking the trio down to the wellness garden was no simple task, and she knew it was asking a lot of her staff in already demanding circumstances. They helped shuffle doctor and therapy appointments, hours-long wound care treatments, and food services so not even a meal would be missed. The nurses covered the firefighters thoroughly so the sun couldn’t irritate their burns further. Hall and Gadomski both had bulky external fixators to keep their leg bones aligned, so several staff members had to help hoist them into wheelchairs.
That hour in the garden was the first time the three firefighters had been together since the explosion. More hardships were yet to come—infections, surgeries upon surgeries, physical therapy sessions so painful it made death seem easy—but there beneath the open sky, existence itself felt extraordinary.
“The fact that I was walking myself down there, and I was outside seeing other people, seeing trees, being alive—it was very surreal,” Perez says. “Because a few days before that, I thought I was going to die. I thought my last breath was going to be on that scene.”
Hall asked to be wheeled out under a sunny break in the clouds, even if just for 30 seconds. He spread his arms out wide. “You know, that did me a world of good, just to feel like I’m gonna be able to breathe and feel the sun again one day,” he says.
It wasn’t until later that he realized how much work went into that moment. “That’s a testament to Katie and the staff,” he says. “I think they oughta make a saint out of her.”
Gadomski and Hall returned to jobs with Dallas Fire-Rescue two days before the first anniversary of the explosion. Hall is again working dispatch and swears he’s sticking to a summer retirement date: “It’s going to be hard to leave, but I love my wife and if I don’t retire soon I’ll have to find a new one.” Perez was unable to use her hands for eight months, requiring 24-hour care. In January, she had her 13th post-Parkland surgery, with the goal of thinning out scar tissue to regain mobility. She hopes to bring eyelashes back to Station 25 as soon as possible.
In its 150-year history, the Dallas Fire-Rescue Department has never experienced a disaster of this kind, with their own men and women trapped inside a blast zone. Shockwaves could be felt 6 miles out. After several weeks at Parkland and through months of recovery, many doctors told the firefighters their cases were unbelievable, that the human body was not meant to survive such a disaster.
Yet last September, just shy of a year after the explosion, all three firefighters—Perez, Gadomski, and Hall—stood in their dress uniforms to receive Star of Texas awards in Austin. Mapula was there to see it.
This story originally appeared in the March issue of D Magazine with the headline, “Team Up.” Write to [email protected].
Author