Years ago, when a woman had breast cancer surgery, she would expect to live with either one or no breasts. Alternatively, she had the option to undergo extensive breast reconstruction, which often had poor results. Current advances in all aspects of breast cancer treatments and breast reconstruction have helped women with breast cancer live longer and with better outcomes. Breast cancer treatment previously focused on surgery alone, removing the breast, muscle, and lymph nodes. As the field evolved, there has been an acknowledgement that the breast is closely tied to femininity, and preserving natural appearance of the breast is an integral part of treatment. “Surgical techniques available today allow women to wake up after surgery feeling much closer to their pre-surgical state,” says Rachel Warren, M.D., a fellowship-trained breast surgical oncologist with Texas Breast Specialists. “This allows patients to have a more positive experience as they navigate treatment and recovery.”
Dr. Warren commonly uses a hidden scar approach in breast surgery. This involves operating from more aesthetically pleasing locations, such as a natural fold in the breast or around the areola when appropriate. She often performs lumpectomies with local tissue rearrangements to preserve shape of the breast and works with a plastic surgeon, combining her tumor removal surgery with a plastic surgeon’s oncoplastic techniques to lift and reduce the breast. For mastectomy patients who qualify, Dr. Warren can perform nipple-sparing mastectomies that allow for nipple preservation. Tissue-based reconstruction has improved significantly, giving women after mastectomy options to avoid implants. “Current breast cancer surgery techniques focus on ways to decrease surgical interventions without compromising oncological outcomes,” Dr. Warren says. “Most surgical advances that have been made have breast surgeons asking the question, ‘Is more surgery really better?’ Research is allowing us to reduce negative surgical outcomes, such as lymphedema, by performing targeted surgical approaches when applicable.”
Dr. Amelia Tower, a fellowship-trained breast surgical oncologist with Choice Cancer Care, was among the first surgeons in Dallas to become hidden scar certified. In some cases, her patients look as if they never had breast surgery, even though it was a critical surgery needed to remove a cancerous tumor. “Some patients can have a mastectomy and breast reconstruction in one day,” Dr. Tower says. “This has been a game-changer for women because everything is done at once, removing the anxiety associated with the constant reminder about breast cancer.”
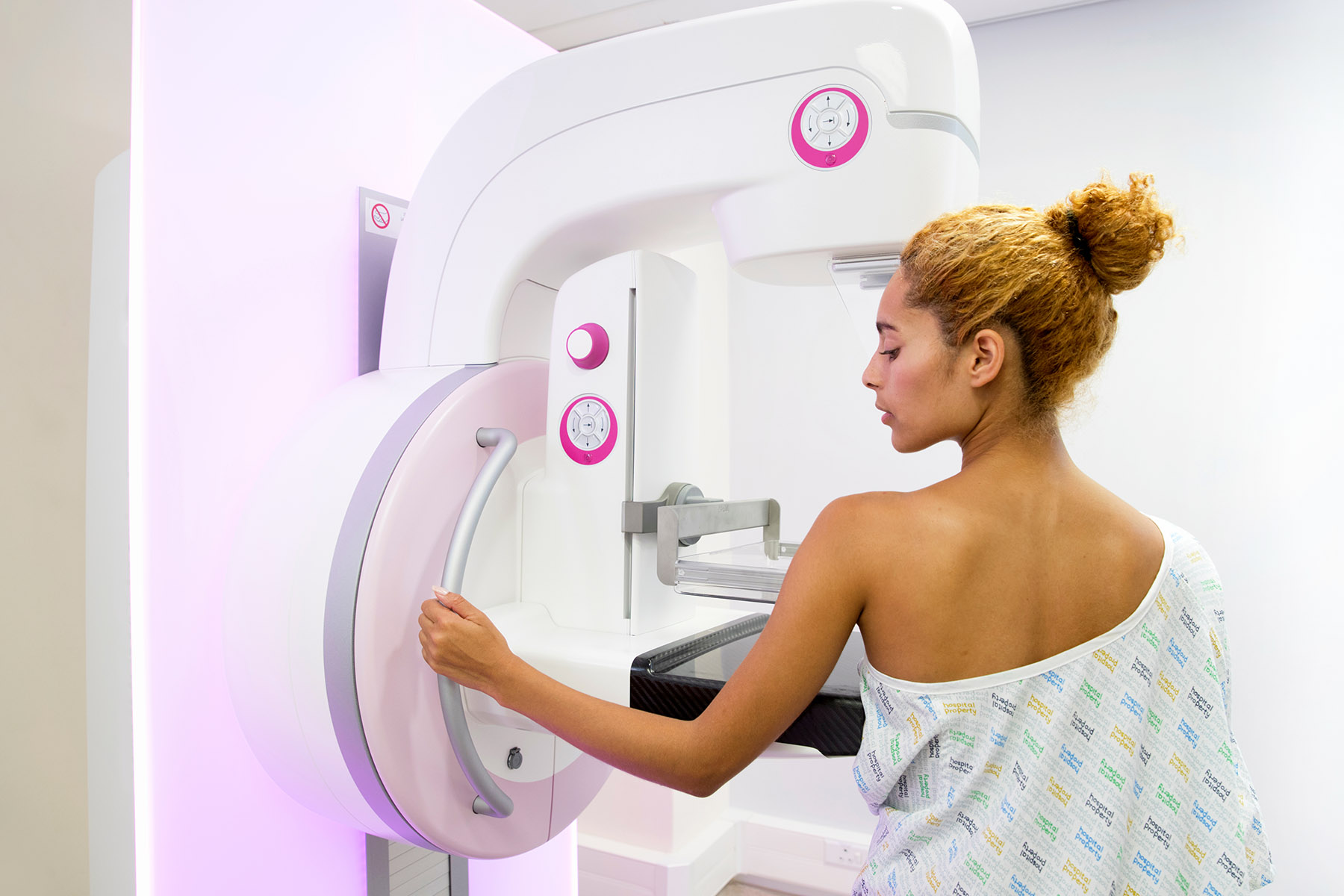
The earlier cancerous cells and tumors are found, the more likely breast cancer treatments will be effective. Therefore, mammograms remain the preferred method of breast cancer screening. In some cases, mammograms and an MRI are needed for effective screening. When breast cancer is detected early and is in the localized stage, the five-year relative survival rate is high. For women with a direct family history of breast cancer, genetic testing is also a way to measure risk and make decisions about prevention. Newer genetic testing technologies and panels are available, and some insurance companies are now covering cover genetic testing. Most often, women with a parent or one other relative with breast or ovarian cancer or metastatic cancer can get genetic testing covered by insurance.
As a breast specialist, one of Dr. Warren’s focuses is on educating women about how to identify elevated risk and then using strategies to reduce risk or detect cancer at earlier stages. “Many women fall into the category of elevated risk for developing breast cancer,” she says. “Certain factors that aren’t modifiable, such as family history and dense breast tissue, will lead to an elevated lifetime risk of developing breast cancer. Clustering of cancer in the family may lead to recommendation for genetic testing, which has become more affordable and accessible since 2015. Nothing has replaced the mammogram as the gold standard for early detection of breast cancer.”
Dr. Tower is among several breast surgeons in the Dallas to use the FDA-approved SAVI SCOUT® reflector implant for wire-free breast tumor localization. It allows the physician to mark a biopsy or lumpectomy site to precisely target the affected tissue and pinpoint its location, resulting in a more successful surgery for tumor removal and optimized breast conservation. The reflector is smaller than a grain of rice and non-radioactive, and the patient doesn’t feel the reflector regardless of how long it is left in the breast. “A woman can’t always feel an abnormality,” Dr. Tower says. “That’s the importance of a mammogram—to detect the abnormality early. When we place the wire at the site where the abnormality was detected, the surgery is more accurate, and we can remove less tissue. Breast cancer can be a very emotional diagnosis, and advances like this can help, so that a patient knows everything is being done to eliminate the cancer and provide the opportunity for a more natural-looking appearance.”