Over the weekend, comments from a Plano doctor published in the most recent issue of the Dallas Medical Journal elicited far and wide criticism on social media. Answering a question about the gender pay gap among physicians, Dr. Gary Tigges, an internal medicine doc who has a practice in Plano, said the following:
Yes, there is a pay gap. Female physicians do not work as hard and do not see as many patients as male physicians. This is because they choose to, or they simply don’t want to be rushed, or they don’t want to work the long hours. Most of the time, their priority is something else … family, social, whatever.
Nothing needs to be “done” about this unless female physicians actually want to work harder and put in the hours. If not, they should be paid less. That is fair.
Screenshots of the comment on Twitter received thousands of retweets, and the ensuing conversations spanned hundreds of comments. Dr. Faizah Bhatti, a neonatologist in Oklahoma City, called Tigges a “sexist misogynist and a disgrace to our profession” in a tweet, attached to a photo of Tigges’ comment, that was passed around 12,000 times. The story eventually received national news coverage, with outlets from the Washington Post to Fox News to CNN picking it up. On Monday, Tigges issued an apology to all female physicians and to his staff and partners at Plano Internal Medicine Associates, the practice he founded in 1996.
Whether the comments will bring forth any lasting impact for Tigges remains to be seen. The Iowa-born Tigges, who did his internal medicine residency at the University of Texas-Houston, currently chairs the Credentials Committee at Texas Health Presbyterian Hospital Plano. I reached out to Texas Health Resources for comment and will update this story if and when I hear back. On Twitter, the official Texas Health account said that Tigges’ “personal political opinions do not reflect or represent the values of Texas Health.”
In an interview with the Dallas Morning News over the weekend, Tigges said that his “response sounds terrible and horrible and doesn’t reflect what I was really trying to say.”
“Women might take longer with their patients, and that’s a great thing, but then their pay is less,” he told the DMN. “That’s something we have to deal with every day; you have to work out that balance. Every physician wrangles with that. But it was not my intention to say female physicians are lazy or don’t work as hard.”
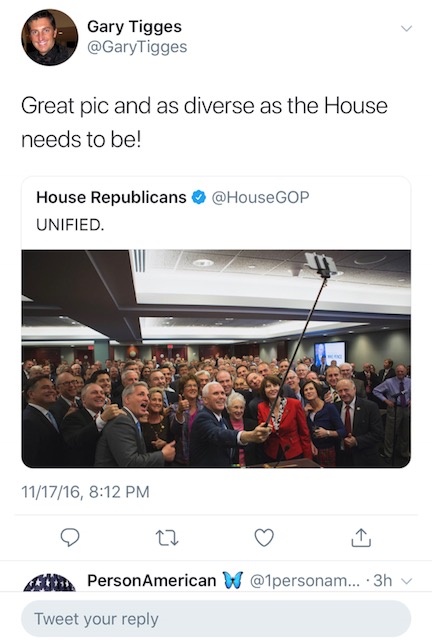
In the online fallout, several Twitter users brought to light recent tweets by user @GaryTigges, an account that used a profile photo of Tigges. On a 2016 photo posted by the official Twitter account of the House Republicans that shows an entirely white assembly, Tigges commented, “Great pic and as diverse as the House needs to be!”
In another, @GaryTigges responds to actress Debra Messing’s quote-tweet of a news article on the Trump administration launching a Denaturalization Task Force, calling Messing “Poor dip-s*** ignorant Debbie,” and imploring her to, “Tell your Mexican immigrant maid hello for me.”
The Twitter account was deleted over the weekend. The DMN’s story doesn’t address Tigges’ apparent Twitter history, and Tigges didn’t respond to a message seeking comment on the matter. Someone called back from his office late Tuesday afternoon, but hung up as soon as the phone was answered.
The Dallas Medical Journal publishes monthly, and its “Big and Bright Ideas” page is a new feature that highlights member physicians’ answers to survey questions. The September issue asked physicians whether they believed a gender pay gap exists, what the causes are, and what steps doctors can take individually and as a community to address the issue.
Dr. Ruben Velez, Dallas County Medical Society president, and Dr. Sue Bernstein, chair of the DCMS Women in Medicine Forum, issued a statement to D CEO Healthcare on Tuesday: “The Dallas County Medical Society believes it would be far more productive to focus this discussion on the problem of gender pay inequities. And make no mistake, it is a problem,” the statement reads, in part. “We hope we can use the tremendous publicity our article generated to find ways to fix the issue we are all talking about: the gender pay gap in medicine.”
The Journal’s spread features a wide variety of responses, with five of them coming from men and three from women. Dr. Shashi Dharma, an ophthalmologist, said that reasons for the gap include “the false perception that women are less efficient, take more time off for family needs, and cannot effectively represent a family practice or institution.”
“The solution is to have transparency throughout the hiring, compensation, and firing processes,” she went on. “Requirements for the job, including nonclinical duties, holidays, coverage, and compensation for both genders, should be clearly and concisely stated in all hiring of physicians.”
Dr. Shaina Drummond, an anesthesiologist, added a lack of mentors, women going part-time more often than men, and the prevalence of male leadership to reasons for the gap. She suggested steps like onsite childcare and making sure women have the same tools for advancement provided to men.
Answers from male physicians tended to focus less on solutions and more on the cause. Dr. Rob Tenery, an ophthalmologist, attributed the gap to hours worked, specialty, and location.
“My guess is that females work shorter hours on average and on average go into specialties that require shorter hours—family practice and psychiatry versus neurosurgery and orthopaedics,” Tenery said. “Also, I believe that reimbursement levels by the payers are based on the diagnosis, complexity and location of procedures or treatments rendered.”
Dr. Bryan Wohlfeld, a neurosurgeon, said that pay within his specialty relates to “hospital need, work productivity, willingness to take call, academic productivity, and subspecialty as some reimburse more/less than others,” and said that the pay gap stems from time away from work “for whatever reason: travel/kids/social lifestyle.”
“I am paid less than many females and males I know, having chosen an academic practice, and more than others who work less or in other subspecialties like meds or peripheral nerve,” he said.
Psychiatrist Dr. Tom Grugle said that white males have traditionally had a “huuuuuge head start and incredible advantage and privilege which they (we) have been loath to give up.” He said that physician leaders should look at pay and adjust accordingly to eliminate gender bias.
You can view the Journal‘s spread in full here.
According to the 2018 Physician Compensation Report published by Doximity and based on responses from more than 65,000 licensed U.S. doctors, male doctors make 27.7 percent more than their female counterparts. The overall gap is larger than in any one specialty, which likely means there are more male doctors in higher paying specialties.
But the gap persists, and to a significant degree, across every single specialty, according to Doximity. The gap is least prominent within colon and rectal surgery, where females make $331,000 a year compared to $387,000 for males, a 14 percent difference. The gap sits at 15 percent for pediatric infectious disease, pediatric cardiology, geriatrics, and plastic surgery.
On the other end of the spectrum, the pay gap is the largest in these five specialities: hematology (20 percent), occupational medicine (20 percent), urology (20 percent), orthopedic surgery (19 percent), and gastroenterology (19 percent). Every other specialty has a gender pay gap between 15 percent and 19 percent. In dollars, the largest gap exists in neurosurgery, where male surgeons earn $118,014 more than their female counterparts, according to Doximity.
In Medscape’s 2018 Physician Compensation Report, male primary care physicians were found to make an average of $239,000 last year compared to $203,000 for their female counterparts, a difference of 18 percent. That compares to 16 percent in 2016. Among specialists, men made an average of $358,000 in 2017 compared to $263,000 for women, according to Medscape, which didn’t break out the pay gaps by individual specialty.





