By the end of 2022, many employers had become aware of quiet quitting, with burned-out employees working just enough to meet standards. Less discussed were those at the other end of the spectrum—the workers who were going and beyond to positively impact their organizations. Healthcare workers often have a natural high-achieving mindset as healers and helpers. For example, Dr. Robert Fine, director of ethics and palliative care at Baylor Scott & White Health, has worked on establishing field-defining, end-of-life care policies since he was a grad student in the 1980s. Chief Nursing Officer for Medical City Arlington Jim Allard educates politicians on how policy affects those in the field. And Dr. Danny Holland left the U.S. to serve as medical boots on the ground in Ukraine.
These individuals and the other 64 leaders and organizations honored in D CEO’s 2023 Excellence in Healthcare Awards are among overachievers in the field shaping healthcare through policy, advocacy, and community work. These extraordinary professionals help make North Texas one of the most successful healthcare markets in the U.S.
Early experiences set Dr. Fine on a mission to improve the ethics of death and dying, and his pursuits have led him to the heights of advocacy and thought leadership. After medical school at UT Southwestern and residency at Baylor University Medical Center, he found that treatment for those at the end of their lives was borderline unethical.
He remembers doctors talking about how they would react slowly if a very sick patient went into cardiac arrest to avoid futile resuscitation. In other instances, physicians performed life-saving measures on patients who had passed away hours earlier. Back then, “do not resuscitate orders were rare, so it was protocol for hospital personnel to go through the motions of CPR on a patient who had been dead long enough for rigor mortis to set in. “This was distressing for everybody involved,” Fine says.
At Baylor in the 1980s, he worked to diversify the ethics committee to include nurses, social workers, and community members who could bring new perspectives to end-of-life care. “How can we say we’re an ethics committee when the only people in the room are the physicians, the lawyer, the administrator, and the chaplain?” he says.
Fine later helped craft the language for rules written into the Texas Advance Directives Act of 1999, which has informed other states on how patients should be able to establish end-of-life instructions ahead of time. Less than 10 years later, palliative care received its board exam partly because of his efforts and thought leadership on the topic. Fine was also one of 17 national task force members who determined the content of the new clinical ethics certification.
He has published countless works and served on numerous federal and state committees around palliative care, but what started him on his journey to thought leadership were memorable interactions with individuals. He remembers one patient, whose life he helped save, telling him staff should not have saved his life. Fine was upset and initially thought the patient was ungrateful. But he soon changed his tune. No one had asked the patient about his limits or principles, and there weren’t policies to ensure that wouldn’t happen again. “These are the stories that led to the direction my career is gone,” Fine says. “I got serious about medical ethics.”
Educating Lawmakers
In high school, Jim Allard often left during the day to work with the local ambulance service in Yarmouth, Maine. As a certified ambulance attendant, he’d raced out of class after receiving a call on his radio to join the EMTs. These early experiences exposed him to the inner workings of the healthcare industry and fostered a desire for healing and effective policy that continues to this day.
Now, as chief nursing officer at Medical City Arlington, Allard serves as a legislative advocate in Austin, speaking to lawmakers about healthcare and the challenges nurses and other caregivers face. He has also been to Washington, D.C., representing Medical City’s parent company where he spoke about workplace violence, the nurse education shortage, and increasing funding for vulnerable populations.
In 2014, Allard was part of a steering committee addressing fatigue in nursing, and he advocated for changes that would improve nurse retention. He has also been to the Texas capitol on Nurse Day at the Capitol as a representative of the Texas Nurses Association. “We used our experiences and opinions and spoke to legislators and educated them about what is important to nurses,” he says.
Although Allard was initially intimidated by approaching lawmakers, he found that they were more receptive to his message than he thought. The nurses were the experts on the issues faced by frontline caregivers, and were able to impact policy. Allard points to his work with advocates this year pushing for bills meant to protect healthcare workers after a horrific shooting at Methodist Dallas Medical Center as his most impactful achievement.
Between legislative sessions, Allard crafts position statements on possible future topics, such as giving full practice authority to nurse practitioners. “To those who say they aren’t going to vote and that voting doesn’t matter, my response has been to educate politicians about how to vote on a topic,” he says. “I encourage other people to go for it. It matters.”
In the Midst of War
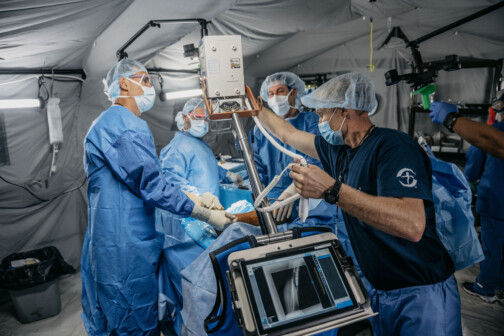
When Dr. Danny Holland landed in Izyum, Ukraine, in October 2022, he found a devastated city without healthcare services in the midst of war. He arrived at a three-story shopping center that had been turned into a makeshift hospital and dormitory for him and the other Samaritan’s Purse volunteers after the city had been targeted and bombed by Russians.
Driven by his faith and feeling called to serve where he could, Holland put himself where few ventured. For the next month, he and a team of international medical volunteers treated the sick and wounded in Izyum, where they could see the firefights and smell the scent of war. Residents who were unable or unwilling to evacuate had lived without healthcare, relying on the hospital and volunteers to treat neglected ailments and injuries from everyday life as well as missile attacks.
Holland and the team provided round-the-clock care to victims of land mines, military battles, and untreated chronic conditions. Team members also donated their own blood along the way, in the hope it could be used to save a life. Holland had been on other medical mission trips to Africa, but the unpredictability and danger in Ukraine were new to him. “Just knowing what those people were fighting for out there, giving everything, was difficult to think about for me,” he says.
The team could only send the occasional encrypted email to family, which increased the stress level for Holland’s wife and children, who supported his desire to help but also worried for his safety. The month left Holland thankful for the comforts and peace of living in North Texas and gave him a new appreciation for the reality of war and invasion, but the lasting change from the experience came from an unexpected place.
The lack of reliable internet and electronics forced him to get to know the other volunteers and patients in a way that he never did at home. He admits that he was often the stereotypical trauma surgeon, with a “bone broke, must fix” mindset that didn’t leave any room for genuine connection with his patients and coworkers at the hospital—Holland’s time in Ukraine helped him slow down and appreciate the people in front of him.
“Taking care of a patient is a lot more than just a finite technical skill,” Holland says. “You must have the full picture and understand where they’re at in their journey. I take care of a lot of trauma patients, and their life is completely upended in a split second. It’s important to spend that time with them.”
Author








