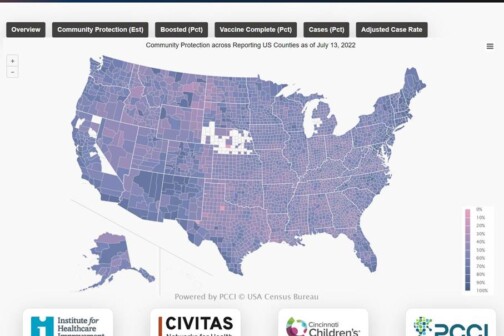
It didn’t take long for the omicron variant to become the dominant version of the disease in the United States. Just weeks after arriving, 73 percent of all new cases sequenced are now omicron. It will soon be the dominant strand in North Texas. But as hospitals prepare for yet another wave of COVID patients, there may be a silver lining to the highly contagious variant.
According to the World Health Organization, cases are doubling every 1.5 to 3 days. The delta variant doubled cases every seven days. But it isn’t all bad news when it comes to omicron. Bloomberg News reported that only 1.7 percent of identified Covid-19 cases resulted in hospitalization during this fourth wave, compared to 19 percent of cases during the delta wave.This week, Harris County reported the first death related to the omicron variant in a man who had been previously infected. According to a statement from the Harris County Health Department, he was unvaccinated and had underlying health conditions.
In North Texas, hospitalizations are staying steady, with about 800 patients across all of Trauma Service Area E, which includes 19 counties in the region. Dallas County has chosen to keep its advisory level at “orange,” which recommends residents use “extreme caution” when venturing out of their homes. Dr. Philip Huang, Dallas County’s health director, told county commissioners on Tuesday that omicron’s rapid spread is “very scary.” About 56 percent of residents in Dallas County have received both shots of the vaccine.
But DFW Hospital Council President and CEO Steve Love says hospitals are preparing for another surge, especially if the region follows the patterns set in the U.K. and South Africa. However, we can do things to help alleviate the pressure on providers.
“We anticipate that a lot more people are going to want testing,” Love says. “Many may come to emergency rooms, but if they’re only coming in just to be tested, it’s probably better to go to a community testing site.” Emergency rooms are trying to treat people to keep them out of the hospital, and testing will delay that treatment, which could keep the hospitals from being inundated.
As of Tuesday, hospitals in North Texas are running at 92 percent capacity, Love says. Only 5 percent of those cases are COVID-19, which is much lower than during previous stages, when around a quarter of all hospitalized patients were sick with COVID-19. But another surge could result in capacity issues.
The primary concern isn’t bed space, Love says. Staffing the hospitals will be the most significant challenge. Local hospitals are already employing traveling nurses to staff their current beds, and a rush of omicron cases would deplete an already exhausted workforce. As vaccine protection wanes, Love said he is also concerned about hospital staff becoming infected, exacerbating existing shortages. Reuters reported that in the U.K, two vaccine doses were 0 to 20 percent effective against omicron, while a booster pushed that immunity from 55 to 80 percent. The odds of reinfection are 5.4 times higher for the omicron variant compared to delta. Past infection may only be 19 percent effective in preventing omicron.
Love says that some facilities are looking at changing the isolation and testing protocols for healthcare workers to deal with shortages. If an employee tests positive, hospitals could reduce the isolation time following a negative test to return to work. The National Football League recently revised its COVID-19 policy to get players back on the field quicker after a positive test if they are boosted and don’t have symptoms, and healthcare could be forced to make a similar move.
There could be a silver lining if omicron proves to be more contagious and less severe (but there is divided data on that conclusion). Much like the 1918 influenza moved from pandemic to endemic that we live with today, omicron could be what triggers a similar shift by quickly wiping out other more dangerous variants. There is precedence. In 2009, Swine Flu took out other flu viruses for years but was a very mild infection. This would be an ideal path for COVID-19. A highly-contagious but mild version of the virus can be managed with treatment and vaccines and could eventually become a seasonal virus like the flu.
That said, the more the variant reproduces, the more likely a mutation will occur. The next variant could be more severe or less resistant to treatment and vaccines. But compared to this time last year, we are in a much better position, Love says.
“I’m not minimizing, and you can still die from it. It’s still very serious,” he says. “You may end up in intensive care or on a ventilator, but I think we’re in a much better position from the point of treatment protocols and vaccination rates. That will help us be much better prepared this year than 12 months ago.”
Author