Patients spend much more time with nurses than they do doctors. Lucky patients spend their time with the nurses whose work has earned them kudos in our fourth Excellence in Nursing Awards. (For the full list of finalists, go here.)
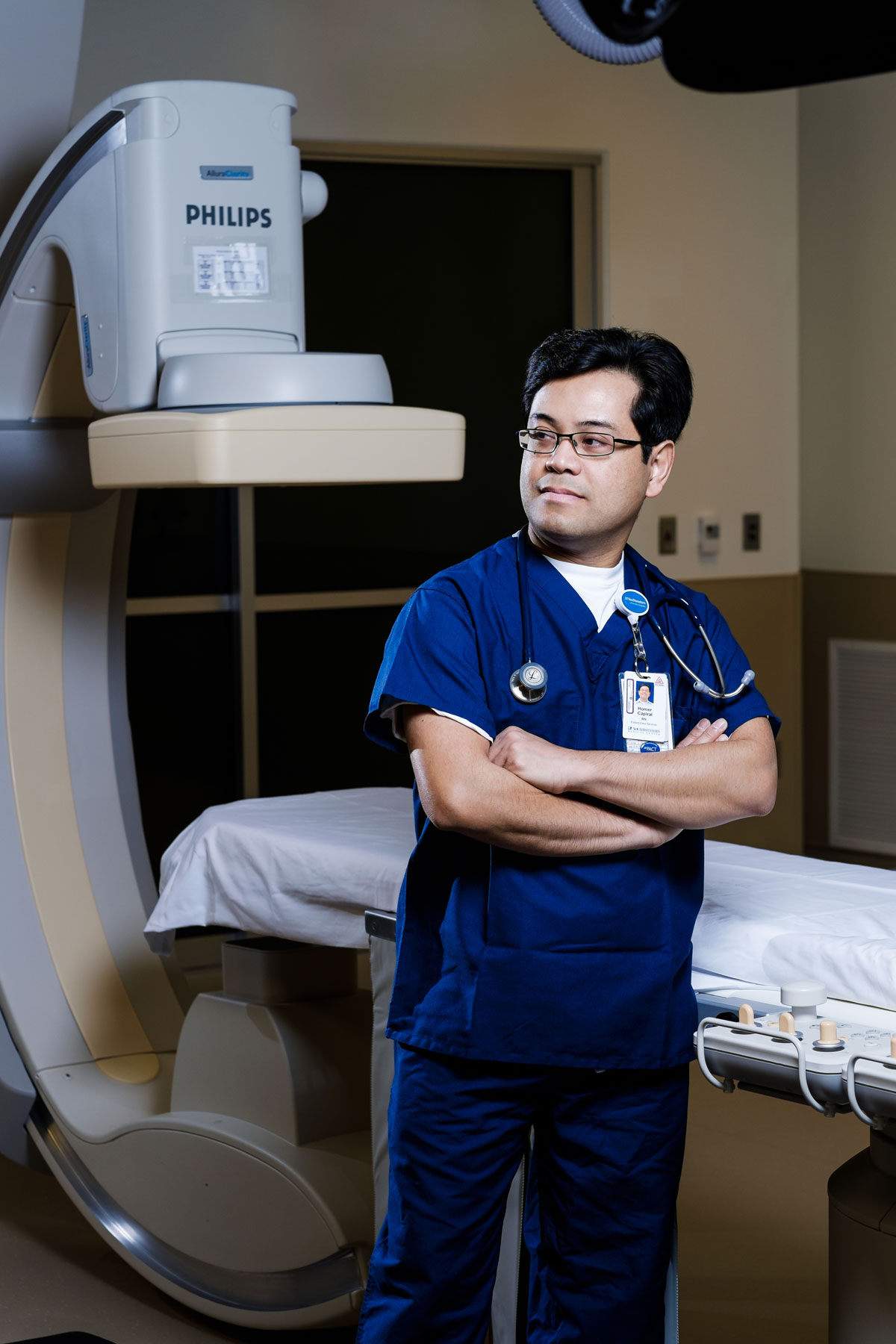
Homer Capiral
Cardiovascular
Homer Capiral’s mother is a nurse, which is only part of the reason he went into the profession. “I love interacting with the patients,” he says. “It gives you a sense of accomplishment and a sense of worth when you see them at the time that you took care of them to a point that they get well and get discharged.”
Capiral is the assistant manager for the cardiovascular and interventional radiology labs at UT Southwestern Medical Center, where he guides the workflow for 10 labs and 25 staffers. The hospital’s Interventional Radiology Clinic uses the latest imaging technologies to diagnose and treat cardiovascular disorders without open surgery.
But when major surgery is required, Capiral is there. He once had a young patient who was brought to the hospital in heart failure. “It was a life-or-death situation,” he says. Capiral stayed with that patient in the cath lab, throughout the emergency procedure, and in the ICU. The patient survived and eventually received a heart transplant.
His caring extends to his fellow nurses. In 2009, Capiral—whose family is from the Philippines—got involved with the then struggling Philippine Nurses Association of North Texas. Under his leadership, the organization has grown to include continuing education programs as well as provide a welcoming space for nurses who have only just arrived in the states.
Jackie Cox
Emergency
When Jackie Cox found out she had Stage 3 colon cancer in January 2011, she made a choice. “I decided that cancer is one word, and it didn’t define me,” says Cox, director of emergency services at Lake Pointe Medical Center. After her diagnosis and throughout her 10 months of treatment, Cox—a single mother of two boys—missed just one day of work, and that was for surgery to remove the tumor.
She has long known the importance of simply being there. By the time she was 17, Cox had become the caretaker for her mother, who suffered from Alzheimer’s, and her father, who was battling cancer. “So I’ve always included caregivers in the patient’s care,” she says, “and treated them with the same respect I was treating the patient.”
Cox extends the same courtesy to her staff, which has grown from 35 to 115 since she took over the director role six years ago. In that time, she has helped Lake Pointe gain notable clinical certifications and overseen expansion projects that include an urgent-care center and two freestanding, fully functioning emergency departments.
“As a director, you get to impact every single patient that walks through the doors,” Cox says.
Michael Munger
General Practice
One Saturday last March, the chronic back pain that had crept into Michael Munger’s life over the past 18 months worsened, leaving him couch-ridden in his Las Colinas home overlooking Lake Carolyn. Not long after taking his meds and settling in for the afternoon, Munger heard a cry. He pulled himself to the window and saw a set of small arms above the water.
“There’s nothing worse than the feeling of a limp child in your arms,” says Munger, a certified registered nurse anesthetist at UT Southwestern Medical Center. Munger went into “adrenaline mode,” rushing to the lake and saving the unsupervised girl.
Munger, who served as a junior firefighter in his teens, has plenty of experience with emergency rescue. As a licensed CRNA who is also a certified EMT-paramedic, Munger combined these skills to create the first state-certified volunteer paramedic response unit in New York, serving six rural communities before he moved to Dallas in 2013. Munger now brings these varied experiences to his CRNA students. “Learning is a two-way street,” he says. “They learn from me, and I learn from them.”
Jennifer Gray
Educator
It started with a chance meeting in 2005 between the queen of Buganda, a kingdom within Uganda, and Jennifer Gray, an associate dean for UTA’s College of Nursing. During the conversation, Gray happened to mention the work some of her colleagues and Ph.D. students hoped to do in Africa. That led to a lasting partnership. Ten years later, Gray spends three weeks in Uganda each summer, working with the Ugandan Nurses and Midwives Union.
In addition to her international work, Gray, one of the founders of the nursing school’s Ph.D. program, has an extensive background in research and has published her work related to patients living with HIV and AIDS. Gray credits her first trip to Africa—in the 1970s with her church—as a driving force behind her career. “It all came together for me in that experience,” she says, “and that has been something that has kind of guided my work as an educator.”
Rose Montgomery
Long-term Care
In her five years at Whitesboro Health and Rehabilitation, Rose Montgomery has displayed a selflessness that has earned admiration. From working the floor throughout the night to aid her short-handed staff to buying patients things she thinks they may like, Montgomery goes beyond the duties of her position as director of nursing.
For Montgomery, this level of care is second nature. She grew up within the walls of her father’s family practice. She also has a strong personal investment. Her brother Sean was a resident of a long-term care facility for 13 years after sustaining a brain injury in a car accident. About a month after Sean’s death, Whitesboro admitted a young man with a similar injury. But he had a different outcome.
“I was able to see that young man walk out of the facility, and to this day, he comes and visits me from time to time,” Montgomery says. “He was, and still is, truly a blessing to me.”
Sara Wick
Geriatrics
When Sara Wick realized one of her elderly patients was continuing to bake pies in her small South Dallas home—in the summer, without air conditioning—she stepped in and anonymously donated a window unit left over from a recent remodel to her church. The woman’s insistence on continuing with her routine might sound frustrating to some. But that kind of independence and tenacity is what initially attracted Wick—a gerontological nurse practitioner at Parkland Center for Internal Medicine—to geriatrics. She was one of Parkland’s first nurse practitioners in the mid-1980s and sits on Dallas’ Senior Affairs Commission. She has spent the majority of her own career lobbying and caring for the elderly.
“I’ve always had the idea that we need to do something to make the quality of life as important as the quantity of life,” Wick says.
Susan Smith
Adult Intensive Care
Over the course of her 30-year career, Susan Smith has practiced nursing, taught college students, conducted research, and published pieces in nursing journals. Recently, the clinical nurse specialist found the time to go back to school. “I think the one thing I’m most proud of is that I never sit still,” Smith says.
The 118 beds in her critical-care department at Baylor University Medical Center keep her busy. But Smith is never busy enough or content to do things the way they’ve always been done. For example: as co-investigator of a study, she was responsible for the implementation of a program for ventilated patients, something that required convincing a lot of different people to try something new. There’s data that show the program is working: patients are spending less time on the ventilator, and mortality rates have decreased.
“My job is to think outside the box,” Smith says. “And not be the one that’s inside the box. Sometimes that’s uncomfortable and difficult for people. You might offend some people, but it’s how you do it that gets people to realize that you’re on their team.”
Sobha Fuller
Community Health
Sobha Fuller may hold the title of pediatric director of nursing, but she’s never considered herself a “behind-the-desk type of nurse.” She started out as a pre-med student but soon realized that nursing was her calling. After obtaining her LVN and RN licenses, she started at Parkland, where her mother was also a nurse.
Fuller now oversees the pediatric and family clinical nursing practice at 12 community-oriented primary-care health centers and 12 school-based health centers, as well as Parkland’s homeless outreach program. She helps coordinate walk-in vaccination clinics and community health fairs, and also assists in emergency situations.
“What I really love is to be on the floor with the nurses,” Fuller says, “seeing how they feel, and working with the patients. I love doing that.”
Kathy Terryah
Cardiology

Terryah is now her medical, surgical, and telemetry unit’s charge nurse at Texas Health Harris Methodist Southwest. She has also chaired the hospital’s Quality and Patient Safety Committee for four years, as well as her unit’s Care Innovation Transformation team. Processes that her team pioneered were implemented hospital-wide. Her 40 years of experience have taught her to look beyond the task in front of her and see the patient.
“Did we connect with them? Did we know their story?” Terryah says. “Healing involves more than just medication.”
Elizabeth Mathew
Surgery

“I was upset that day, but it made me even stronger,” she says. “I have to take my emotions and help more people. Because my mom will be happy if I’m saving more lives.”
Kathy Rose
Hospice
Kathy Rose never intended to be a nurse. She was taking a semester off from her physical education studies when her best friend announced she was signing up both of them for nursing school. So she went along with it. “Forty-one and a half years later, and I can’t imagine doing anything else,” Rose says.
The bulk of Rose’s early career was spent working with newborns and new moms, teaching childbirth classes and breastfeeding. After two decades, her professional focus flipped from helping parents welcome new life to helping them face the end, as the lead pediatric hospice nurse for Community Hospice of Texas.
“To me, whether it was teaching mother/baby classes or telling somebody about hospice, it’s all about empowering parents to be the caregivers and give them control,” she says. “Because when someone’s child has cancer, they have no control.”
When she visits a patient’s home, she isn’t there to take over but rather to help—to ensure parents have Tylenol on hand in case of late-night awakenings, and that they know how to change out the feeding tube.
“There’s nothing better than a parent feeling confident and competent that they can take care of their child,” Rose says.
Heather Paterson
Palliative Care
At least a couple nights a month, you can find Heather Paterson singing with her jazz quintet, Straight Ahead. She studied music at SMU but went back to school for nursing when her mom got cancer and she decided she needed something more reliable than gigging in nightclubs. Paterson has held her day job for 33 years, and says both worlds, the musical and the medical, require a certain amount of introspection and sensitivity.
But those qualities are surely more in demand in the palliative care program at Children’s Medical Center of Dallas. Her job is to provide comfort and minimize suffering for kids with chronic illnesses, life-altering injuries, and terminal conditions. Sometimes she is helping kids discover a “new normal” as they return to school with complicated healthcare issues. But often, Paterson is guiding families as they make difficult decisions at the end of their child’s life. Will their child die in the hospital or at home? Will they live with the aid of a machine, or is that just suffering?
“If being able to talk about it means that one more person can die with dignity and without fear,” she says, “then I think it’s been a successful conversation.”
Michelle De La Cruz
Orthopedics
Weeks before Michelle De La Cruz became the first nurse practitioner in orthopedics at Baylor Medical Center at Carrollton, she was already brainstorming ways to improve the department. Length-of-stay statistics weren’t even close to the nation’s top programs. So De La Cruz set some benchmarks for care. Joint replacement patients should be helped out of bed on the same day of surgery, for example, which physically and mentally prepares them for the hard work ahead. It’s all detailed in a guide she created for nurses and physical therapists. In the year and a half since De La Cruz took her position, the program reduced its length of stay from four days to about two and a half for knee and hip replacements and received joint certification in both procedures.
De La Cruz’s ambition extends beyond her orthopedic duties. In lieu of gifts for her youngest son’s birthday, she asks friends and family to donate to a cause. One year, she collected 325 pairs of shoes. Her two teenagers passed them out to kids at an orphanage during their annual trip to visit family in the Philippines.
Natalie Moon
Nurse Practitioner–Primary Care

She now works in neurosurgery at Methodist Dallas Medical Center, where her skills were put to good use shortly after taking the job. Her dad was having trouble completing math equations, which was strange for a lifelong accountant. She performed a neurological exam and noticed he had a very slight right-sided weakness.
It turned out to be a blood clot. Her new boss, Dr. Richard Meyrat, performed the life-saving surgery.
Kendel Richards
Pediatric Intensive Care

“It was a very peaceful, very beautiful thing,” says Richards, a nurse in the pediatric intensive care unit at Children’s Medical Center of Dallas. “That’s part of ICU nursing. Sometimes your patients are going to pass away, and it’s not fun. But if you can help the parents go home feeling at peace instead of wondering if they did everything, I think that’s the most you can ask for.”
Mary Robinson
Leadership
Mary Robinson always has a pair of clean scrubs in her office. Her colleagues mention this because Robinson is the chief nursing officer responsible for patient care and all aspects of the nursing services at Texas Health Harris Methodist. She doesn’t need to wear them—ever. But Robinson has been known to make a quick switch to assist the nurses when they are short-staffed, even if it’s the middle of the night as she’s making her frequent rounds. Robinson’s colleagues are full of examples of her character. She goes by Mary instead of Dr. Robinson. She knows most employees by name. They often see her at after-hours functions and running in fundraising races. She has personally mentored 20 nurses pursuing master’s degrees. So it comes as no surprise that nurse satisfaction has gone up every year since she took the job.
“We’re really hitting a lot of our goals,” says Robinson, whose daughter is a nurse and whose mother is a retired nurse practitioner. “And I believe strongly that that happens when you have staff at the table helping to make decisions.”
Maggie Smith
Psychiatric
After a patient injured herself with a pencil, nurses in the psychiatry unit were told to confiscate all items aside from clothes from every room. Management’s definition of contraband included picture frames, makeup, even watches and clocks, the lack of which made psychiatry patients all the more disoriented. “It seemed that we were magnifying their losses rather than helping them overcome their sense of powerlessness,” says Maggie Smith, a staff nurse at UT Southwestern Medical Center’s Zale Lipshy University Hospital.
The policy, she says, affected the entire atmosphere of the unit, pitting nurses against patients and dividing the nurses themselves. So Smith, a nurse for more than three decades, helped find a middle ground, reading through literature and contacting other psychiatry facilities. Once Smith and the team established a new policy, some of the more harmless items were returned to rooms.
“You lose so much control that empowering people—giving them back control and gaining their trust—is a big part of what we do in psychiatry,” Smith says.
Jennifer Hoeft
Neurosurgery

An acute-care nurse practitioner in neurosurgery at Parkland Hospital, Hoeft has been known to spend long hours mentoring nurses, helping a brain cancer survivor get psychological treatment for depression, and ensuring that patients, many of them homeless, are discharged safely. A self-described adrenaline junkie, she always had a passion for working in trauma, but neurosurgery was a different story.
“I knew nothing about neurosurgery, and it scared me,” Hoeft says. “It was just one of those things where I needed to conquer my fears.”
Patricia Kelly
Research
Patricia Kelly combs through stacks of medical journals, stays up to date on the latest research by attending conferences and webinars, and—her favorite part—works directly with the bedside clinical nurses to figure out how they can improve patients’ outcomes. The description of her job is only slightly shorter than its title: Texas Health Presbyterian’s research and evidence-based practice translationist and genomics consultant.
Some studies are initiated at the suggestion of concerned nurses. Others are practice projects launched to keep up with the latest research. For example: recently she educated nurses on decibel levels in the medical intensive care unit, creating a simulation room for them to listen like a patient, and showing them how to adjust volumes and alarm settings to reduce noise (and thus, anxiety). “We are really interested in improving patient outcomes and doing it in a way that is based on science and literature and the best evidence,” Kelly says. “So when patients are admitted, they know that they’re getting the best care possible.”
Purity Nyaga
Home Health
As the clinical director of Methodist Health System’s accountable care organization, Purity Nyaga is in charge of Dallas’ first Medicare Shared Savings program. She was tasked with putting all the clinical programs and processes into place, reviewing the 235 healthcare providers who have joined the network, and hiring and training the care navigators who work with some 15,000 Medicare patients.
While Nyaga directs her team as they check on patients’ health through calls and home visits, she is also looking at the root cause of chronic illnesses. During home visits, care navigators were finding that many patients ate low-quality food. Give a dialysis patient a diet of high-sodium canned goods, and he is likely to end up in the hospital. Last year, she initiated a partnership with the North Texas Food Bank to deliver food to qualifying households and to host a monthly food drop in the Methodist parking lot. October’s drop distributed 6,000 pounds of mostly organic produce to 500 families. Nyaga also invited diabetes management and food stamp programs. “It’s a blessing to see people come and get what they need,” Nyaga says.
Mona Cheung
Neurology
“Partnership” is nurse practitioner Mona Cheung’s most frequently used word, because she needs her patients with epilepsy to help take care of themselves in order to stay seizure-free. “You have to empower them to help themselves,” she says, “and also help us manage their disease more effectively.” Before taking her position at UT Southwestern Medical Center in 2012, Cheung didn’t know much about the neurological disorder. But she has been amazed to see what today’s medications and technology can do to keep seizures at bay, or even cure patients completely. She encourages patients to reinvent themselves, pursue new educational opportunities, or find a job that allows them to work from home.
“I want them to be productive. At the end of the day, that’s the goal,” Cheung says. “Nobody wants to be disabled. Nobody wants to sit at home and do nothing.”
Tamara Holt
Nurse Practitioner–Acute Care
Tamara Holt started off as a nurse in the ICU, then became Texas Health Presbyterian’s first acute-care nurse practitioner in 1997. No one knew quite what the role meant. But Holt was up to the challenge.
Her day starts at 7 am in the ICU, where she meets with four of the six surgeons she works with daily in the first hour she’s on duty. They divide the work, and she starts what she calls “the conquering process.” By 11:30 am, she has made it to every patient on her floor, all while fielding calls and pages. She takes care of everything a cardiothoracic/vascular surgery patient might need, barring a major medical emergency that requires “a fellow with a scalpel,” so that surgeons in the OR aren’t interrupted.
Over the course of her 27-year career, Holt has had the opportunity to impact the medical community in other ways. “Many of the nurse practitioners here in Dallas were once under my wing,” she says. “I’m proud to say that.”
Shanna Atnip
Women’s Health
After three years of active duty as a nurse in the Air Force, Shanna Atnip joined the reserves and headed for Austin. She couldn’t find a job, so she and a girlfriend drove up to Dallas, where she interviewed at Parkland. Thirty years later, Atnip is still there, serving as a women’s health nurse practitioner and directing the hospital’s program in urogynecology and pelvic-floor rehabilitation.
Atnip, who retired from the reserves in 2005, is the leader of the Society of Urologic Nurses and Associates and serves on its board of directors. She heads up research projects with nurses from all over the country, trying to develop a consensus on how to treat women with pessaries, devices that hold up the vagina and the uterus. As medicine becomes more specialized, Atnip says, pessaries are especially useful for nurse practitioners in rural areas, where there aren’t specialty practices.
“I remember a woman the other day,” Atnip says. “I did a pessary for her. She cried and said, ‘You just don’t believe how my life was. This one little thing has totally changed my life.’ ”
Regina Miller
School Nursing
Regina Miller laughs as she explains that she started off as “just a school nurse” at Walnut Hill and Tom W. Field elementary schools. Now she travels around the Dallas ISD to help and educate nurses at countless other schools. From scraped knees to assisting Child Protective Services, every day in Miller’s world offers something new. And then there was the memorable day 13 years ago when a woman ran into her school after her husband had collapsed behind the wheel at a nearby intersection.
“I know all schools have a nurse,” Miller recalls the woman saying, “and I don’t think he’s going to make it to the hospital.” She raced to the scene and performed life-saving CPR on the driver, grateful for muscle memory and her past experience in Parkland’s ER. Miller, who has been with DISD for 18 years, says most district nurses have backgrounds in ER, trauma, or the ICU, and that knowledge base helps them make emergency decisions every day.
“Sometimes I think things like that happen to help us as nurses, to remind us why we got into this in the first place,” she says.
Erica Vance
Pediatrics
Erica Vance isn’t just a nurse. For families, she’s a lifeline. She’s a care coordinator in Complex Care Medical Services at Children’s Medical Center. The hospital pairs nurses with chronically ill children and their families to coordinate, educate, and implement care. Sometimes that means coordinating an apartment relocation for a wheelchair-bound patient. Sometimes it means scheduling eight appointments with eight doctors in one day so parents don’t have to worry about taking another day off work, or staying on hold for three hours to refill a prescription. Vance is there to alleviate some of the stress that comes with having a sick child—being a caregiver rather than a mom or dad. Most often, she finds that the patients’ mothers just want to be moms again. And by taking over tasks like communicating with insurance companies and organizing home medical supplies, that’s exactly what Vance lets them do.
Sandy Lindsey
Oncology
For the past 15 years, Sandy Lindsey has worked with patients in the oncology department at Parkland Health and Hospital. She operates as the chemotherapy infusion center manager, handling assignments, scheduling, and administrative duties. But she also continues to perform patient care services. “My heart is out there with the patients,” Lindsey says. “One-on-one patient care is really what I enjoy most.”
Under Lindsey’s watch, the oncology department has streamlined the patient’s experience from check-in and treatment to discharge. “I love working with people and helping people and trying to make everyone feel better,” she says. “This is a good place to do it.”
Cheryl Riley
Neonatal
As a baby leaves its mother’s body, the placenta continues to pump nutrient-rich blood through the umbilical cord to the newborn. While clamping the cord right away has been the norm for decades, recent research suggests we should all just wait a few minutes. More blood equals more iron. And iron, explains Cheryl Riley, a clinical assistant professor and coordinator of the neonatal nurse practitioner program at Baylor University’s nursing school, is critical for brain development.
Delayed cord clamping is just one of the methods Riley and her team are teaching NICU nurses and rural midwives in India, where up to 80 percent of mothers, infants, and children are iron-deficient and anemic. Riley has traveled to the country three times and is developing a five-year partnership between Baylor and the NICE healthcare foundation in Hyderabad to teach best practices. Their visits have a direct impact on the local nurses as well.
“For women to handle bodily fluids and take care of men is frowned upon,” says Riley, who is also a neonatal nurse practitioner for Sheridan Healthcare. “So when we go there and they see what nurses can be, it empowers them, and it’s really neat to watch them grow.”