Michael Kelly found himself in an emergency department with unbearable shoulder pain. Tests revealed a more serious problem: out-of-control diabetes.
The 50-year-old Kelly, who works part-time for a Dallas pest-control company, knew he was diabetic a decade earlier. But he lacked health insurance to treat it consistently, so he just lived with it.
“I would see a doctor once every blue moon when I had money or I had no choice,” he says. “But I didn’t have money for test strips [for blood glucose] or to eat right. The cost is astronomical.”
Kelly was referred to the Diabetes Health and Wellness Institute in South Dallas. There, clinicians and staff members taught him about proper nutrition and the importance of physical activity, and helped him find affordable medication. With the proper education and tools, Kelly got his diabetes under control in record time, according to DHWI staff members.
He says DHWI saved his life.
“I felt like I was 110 years old. My joints ached. I was stressed out over how I was going to pay my bills. Now I feel like I’m 20 years old,” he says.
DHWI, a collaboration between Baylor Health Care System and the City of Dallas, is just one local program working to curb and help prevent diabetes, which has reached epidemic proportions globally. North Texans have a higher-than-average prevalence of the disease.
DHWI is in the Juanita J. Craft Recreation Center in the medically underserved Frazier Courts neighborhood. It represents a five-year, $15 million investment by Baylor to combat the disease through screening, prevention, and ongoing care. The innovative model of chronic-disease management combines nutrition education, exercise classes, and clinical care under one roof to make diabetes control convenient and affordable.
“In this new healthcare environment, we are putting greater emphasis on prevention and wellness,” says Joel Allison, Baylor’s president and CEO. “We know one out of three Americans will develop diabetes in the next decade, based on current statistics.”
Chronic diseases such as diabetes, cardiovascular disease, and cancers share common risk factors, have lifelong impact, and require organized systems of treatment and active self-management.
DHWI represents an insertion by Baylor into an impoverished neighborhood to forestall chronic disease before it arrives at its emergency-room doorstep. It’s trying to provide screening and preventive care in an area that needs it the most. Less than 43 percent of Dallas area diabetics received recommended preventive care, which is below the national average.

Allison credits the health system’s board of directors, specifically chairman Albert Black, who heads up On-Target Supplies & Logistics. The center’s creation was driven by Black, who grew up in Frazier Courts until he was 14. Since opening its doors in 2010, DHWI has had its intended impact. The center has cut hospital emergency-department visits by 40 percent among the 2,800 center enrollees. Last year, enrollment in the program grew by 28 percent.
Esteria Miller, director of business development, says a key strategy for community acceptance was recruiting 100 church ministers to embrace the center’s efforts. She says church leaders are a powerful influence in south Dallas, and many tied health messages to the scriptures. The center used the network of community churches to recruit and train health workers who assist in the facility’s efforts.
The hallmark of cost-effective prevention is to target those most at risk. The Frazier neighborhood has the city’s worst rates of diabetes, cardiovascular disease, strokes, and cancer. Its average annual household income is about $9,000, compared with more than $42,000 for Dallas overall. Diabetes is a significant economic burden for those who suffer from the disease, because proper self-management requires medication and supplies for monitoring blood glucose. The neighborhood’s diabetes death rate is triple that of Dallas. About 98 percent of residents are black or Hispanic, whose risk of diabetes is nearly double that of whites.
Acting Before Diabetes Strikes
For Sherri Snook, diabetes runs in the family. Her grandfather, mother, and brother all fell victim to the disease. Snook found out during a routine health screening that she was prediabetic. But thanks to a YMCA program, the information technology specialist for a Dallas trade show company has turned the tide.
Snook is taking on-site classes at Freeman, her employer, with about a dozen colleagues. The Y’s 16-week program assists those with prediabetes by counseling them about healthy eating, increased physical activity, and other lifestyle changes. After the 16 weekly sessions, participants meet monthly for up to a year.
The program is part of the National Diabetes Prevention Program led by the Centers for Disease Control. There are nearly 2,700 YMCA facilities nationally; nearly 60 million people—or about 57 percent of Americans—live within three miles of a YMCA location.
When Snook began the class, she weighed close to 200 pounds. Her initial goal was to drop 12 pounds. She has since lost 20, and is on her way to her new goal of 155 pounds. During a recent physical, all of her blood work was normal.
Her weaknesses, Snook says, were hamburgers and McDonald’s breakfasts. Now she settles for Eggbeaters. Her energy level has soared.
“It’s a wonderful program,” she says. “You are trained to watch what you’re eating and to exercise. The ultimate goal is to change your lifestyle.”
The Dallas YMCA, UnitedHealthcare, and local pharmacies launched a program to curb diabetes, prediabetes, and obesity in late 2011. Called “Not Me,” the program is a employer and community initiative. Also available at YMCA facilities in Fort Worth and Arlington, “Not Me” is under way in 48 locations in 26 states. Comcast and UnitedHealthcare are considering creating a “Not Me” reality show on cable television.
North Texas is one of six U.S. locations to participate in the endeavor. It’s an ideal location, as the area has a higher-than-average prevalence of the disease. An estimated 13 percent of North Texas residents have diabetes, compared with 11 percent statewide.
The Y program marks the first time a health plan has paid for evidence-based diabetes prevention and used pharmacists to manage the disease. The goal is for participants to lose about 7 percent of their body weight, cut down on total and fat calories, and participate in at least 150 minutes of moderate physical activity per week. Every two-pound loss lowers the risk of diabetes by 16 percent.
Enrollment is limited only to those with diagnosed prediabetes. Research has shown that the program overall reduces the risk of developing the disease by 58 percent for those with prediabetes. For those older than 60 years, the risk reduction rose to more than 70 percent.
Susannah Peterson, director of health lifestyles at the Dallas Y, says the biggest challenge for participants is realizing that this isn’t a quick-fix weight-loss scheme.
“It takes a few sessions for people to understand that, ‘Oh, this is a lifestyle change.’ We don’t even talk about exercise until the 12th week—other than the number of minutes they need to do—because they get overwhelmed. We spend eight sessions on psychology, or what happens if you fall off the plan. That’s what makes it real, going from short-term fix to long-term sustainability,” Peterson says.
Michelle Mathis, 34, a self-employed disaster-relief field inspector, says she joined the program after seeing it on the Y’s website. She had been diagnosed with polycystic ovary syndrome, which is an imbalance of a woman’s female sex hormones. The condition, left untreated, can lead to diabetes.
Mathis, who lost about two pounds a week, says, “I believe in this program 110 percent. I struggled with balance and sustainability with eating and exercise. I had cut things out of my diet unnecessarily. I am now able to reincorporate things in moderation. And I learned how to do smaller increments of exercise rather than devote two hours to exercise. … I couldn’t wrap my head around how I could devote so much time to it and work full-time.”
Peterson says local physicians have been slow to accept the program because the treatment mindset has been to reach for the prescription pad rather than address lifestyle changes.

About one out of four U.S. adults is prediabetic, although more than 90 percent are unaware of their condition. Those with prediabetes or undiagnosed diabetes without symptoms remain undiagnosed unless blood glucose is measured as part of a routine blood test or complications arise. Of those who have been told they have prediabetes, only one out of three receive medical advice about how to reduce risk factors and the same proportion do nothing to combat the risk factors regardless.
Most of the estimated 67 million prediabetics do not have symptoms and are unaware of their condition. People with prediabetes often have a collection of risk factors, known as metabolic syndrome, that elevate the chance of acquiring diabetes and heart disease. The risk factors include excess abdominal fat, high blood pressure, elevated blood sugar, low levels of good cholesterol, and high triglycerides. About one out of three U.S. adults have metabolic syndrome.
The Prevalence of “Diabesity”
Obesity is so tightly linked to diabetes that its progression has created the term “diabesity.” Risk factors of being overweight and mildly insulin-resistant morph into obesity and diabetes.
One-third to two-thirds of prediabetics will develop diabetes within six years, compared with 5 percent of those with normal blood glucose. About 5-10 percent of prediabetics become diabetic annually. The YMCA’s Diabetes Control Program also offers private, one-on-one consultations with neighborhood pharmacists to help diagnosed diabetics control their condition and reduce the risk of complications such as heart disease, blindness, and limb amputations.
Another area of concern is with Type 2 diabetes. It used to be called adult-onset diabetes. Now, however, it is found in one out of every 2,500 adolescents between 10-19. Physicians are seeing it develop in children as young as 8 years old. Child type 2 diabetes is a function of child obesity. More than one out of six U.S. children are obese, and about 70 percent of those have at least one additional risk factor for cardiovascular disease, such as high blood pressure or high cholesterol. At least 40 percent have two or more.
Of those with type 2 diabetes, about 80 percent of children are obese and 10 percent are overweight. Child obesity is growing three times faster than adult obesity. At nearly $10,800, the average annual child diabetes costs exceed those of adults by more than $2,000 annually.
Child diabetes has a profound effect on education attainment and, consequently, lifetime income. The high-school dropout rate is 6 percentage points higher among those with the disease, and the college attendance rate is 4-6 percentage points lower for adolescent diabetes. They earn about $160,000 less over a career.
Sugar is a major culprit in the onset of diabetes in children. About one out of every six calories consumed by teenagers is added sugar. Most of that sugar is consumed at home, rather than in school or elsewhere.
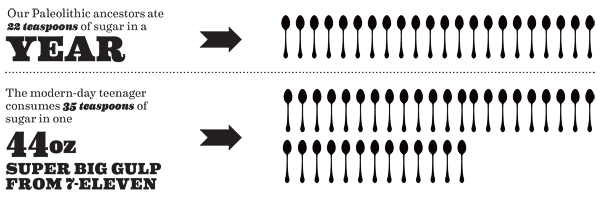
Our Paleolithic ancestors ate 22 teaspoons of sugar in a year. The modern-day teenager consumes about 35 teaspoons in a 44-ounce Super Big Gulp from 7-Eleven. The average American ingests 150 pounds or more in a year. Given that the genetic code is altered .2 percent every 20,000 years, it is clear the human body has difficulty absorbing a daily onslaught of sucrose.
Sandy Peters, associate director at North Texas chapter of the American Diabetes Association and a former physical education teacher, has been educating parents, school personnel, and students about diabetes for seven years. She says it has been an uphill battle to get parents and physicians to recognize the threat of type 2 diabetes in children. She believes the condition is underdiagnosed. “Doctors are reluctant to diagnose it because they don’t want to stigmatize the child,” she says. “And many parents don’t want to hear about it.”
A state-mandated program to determine the risk of type 2 diabetes tells the tale of disbelief. Nearly 9,000 North Texas children had acanthosis nigricans, a dark skin condition that signals high insulin levels. However, less than 100 of those saw a physician for diagnosis. Peters says some physicians referred the children to dermatologists instead of addressing the risk factor.
Research indicates `that for each adolescent diagnosed with type 2 diabetes, there are five others with impaired fasting glucose, an indicator of insulin resistance below the threshold for type 2 diabetes.
Blue Cross Blue Shield of Texas donated $100,000 to ADA earlier this year for the local chapter’s anti-obesity efforts in local schools, including Dallas, Garland and Richardson. Like other programs, the ADA initiative emphasizes a healthy diet and physical activity.
“Type 2 diabetes in children is new to all of us,” Peters says. “It is new for doctors. It is even new to the ADA. Child diabetes was always about type 1 diabetes before.”






