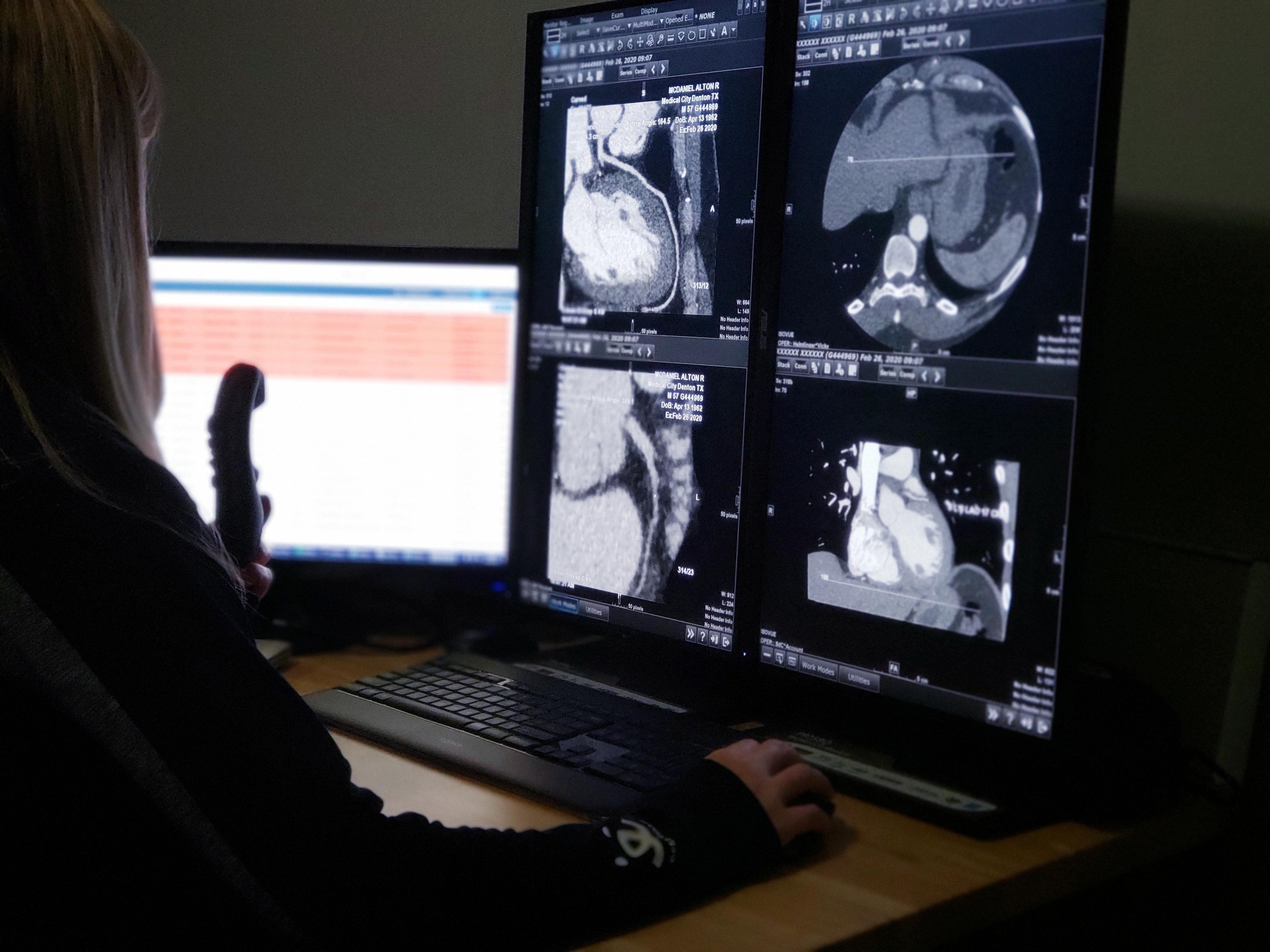
Radiology is one of the specialties most conducive to working from home, and as coronavirus forces providers to avoid close contact, many are making the transition to working from home. But the change is much more than an inconvenient and temporary hurdle – it is improving the accuracy, quality, and speed at which images are being read.
Typical radiology reading rooms have numerous providers and support staff in a small space, so as the social distancing precautions ramped up, radiologists were asked to read images from home. At the same time, elective procedures have dried up all over the country, and much of the work has been shifted to upper respiratory infections and other work connected to the virus.
As the virus squeezes radiology budgets, the groups are looking ways to be more efficient in order to avoid layoffs and furloughs. Collaborative Imaging CEO Dhruv Chopra works with independent radiologists, equipping them with technology and best practices to remain independent. He says he has seen radiology budgets 40-50 percent across the board during the slowdown.
While teleradiology has been around for many years, it hasn’t become widespread until now, mostly because the technology made it difficult to do studies of images from different facilities, which each had their own interface and system. But Collaborative Imaging has enabled its radiologists to be able to read studies at home from any facility.
The quick and pervasive adoption of teleradiology has led to several important changes beyond preventing the spread of COVID-19. The network of radiologists extends from the east coast to Hawaii, which means the ability to analyze images at all hours has extended as well. Hawaii physicians are in the middle of their work day as the rest of the country slows down and heads to bed, meaning the number of radiologists available for nighttime studies has also increased.
The ability to access specialized radiologists has improved as well. When radiologists were confined to one room and not connected via a network, hospitals were limited for the most part to whoever was there that day to read the image. If there was not a neuro or musculoskeletal specialist available at the time, it was up to whoever was on duty to give their best reading. But with radiologists working from home and on a netowrk, a facility can make a request for a specialized radiologist, and the person with the proper training and credentials can step up to read the image, like an Uber for MRIs. “Because we have a network of virtual radiologists, can push that study to the right person,” Chopra says.
Because there is an entire network of radiologists available to hospitals and physicians, the speed at which the studies are being read has also improved. This is especially important as the threat of coronavirus puts different regions in danger. If there is an outbreak in one region of the country that takes out a number of radiologists, healthy physicians in other areas can step up to read the studies and keep the facility running. “The turn around time from the exam to reading the study has gone down dramatically,” Chopra says. “We are ready to jump in and read them very quickly across the board.”
Remote radiology has also allowed practices to reduce their real estate footprint, which is more important as revenue dries up. “With the reimbursement hit and less revenue coming in, we have to cut costs somewhere,” Chopra says. “It is going to be a whole new dynamic as we build up home offices.”
While the circumstances that have served as a catalyst to increased teleradiology are not positive, Chopra sees the improved efficiency and expertise available as an eventual boon to the future of medicine. “The beauty is that while we have been trying to solve a problem we have created a solution to have a much wider range of radiologists that can jump in and read a study,” he says. “We have created a virtual network of our radiologists that gives us the bandwidth to cover each other as we need to.”