When an additional freestanding emergency department (FED) entered a local market in Texas, out-of-pocket costs and emergency provider reimbursement went up 3.6 percent per insured beneficiary, according to Rice University research published this month in American Emergency Medicine.
The study looked at data in four states, but Texas FEDs were especially prolific. The study analyzed 495 Public Use Microdata Areas (PUMA), looking at the number of FEDs in each location and comparing other cost and demographic data. By 2017 there were only 51 PUMAs in Texas without an FED, meaning 74% of PUMAs in Texas had at least one. In Arizona, only 28% of PUMAs had one, 22% in Florida, and 14% in North Carolina had one or more FrEDs.
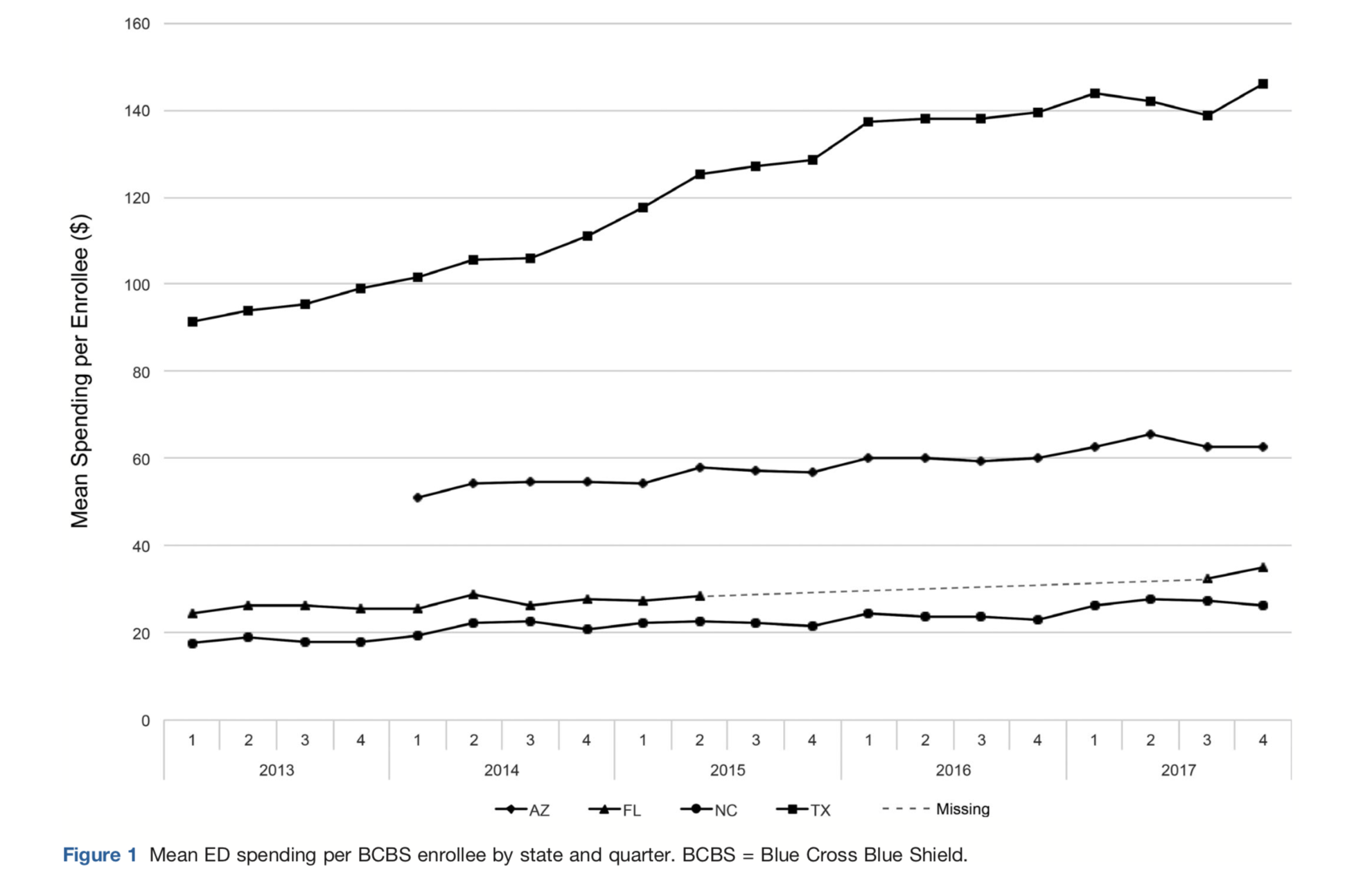
In addition to the growth of FEDs, spending per enrollee was also much higher in Texas than other states in the study. During the four years in the study, spending per enrollee grew from about $132 to $216, and out-of-pocket costs jumped from about $54 to $72. Mean spending per BCBS enrollee in Texas was more than twice as high in Texas than other states in the study.
The healthcare market does not function like a normal one should, and supply often induces demand. The number of hospitals built in DFW over the last decade far outpace the population growth, and “a bed built is a bed filled,” some say. When the added medical facility supply is freestanding emergency rooms, which are almost always out-of-network and more expensive than hospital emergency rooms and urgent care facilities, costs go up. The study found that an additional FED was associated with increased ED utilization in Texas, Florida, and Arizona between three and five percent, but not in North Carolina, where out-of-pocket costs actually decreased 15.3 percent.
“Proponents of freestanding emergency departments claim that these facilities can relieve the burden of overcrowded waiting rooms in hospital-based emergency departments,” said Vivian Ho, lead author and the James A. Baker III Institute Chair in Health Economics and director of the Center for Health and Biosciences at Rice’s Baker Institute for Public Policy via release. “We sought to test whether these facilities increase spending, because they might serve as supplements to traditional emergency departments rather than substitutes.”
Freestanding emergency departments market themselves as convenient alternatives to hospital that help relieve overcrowded facilities and reduce wait times, and are usually located in well-to-do neighborhoods. But they are responsible for a large portion of surprise medical bills, and some facilities have been criticized for confusing signage that have some patients believing they are in network for major insurers. Legislation has moved against these facilities, which represent 83 percent of all out-of-network emergency room services and end up costing Texans more than $3 billion a year in avoidable healthcare payments.
“Consumers mistakenly thought that freestandings would be low-cost because they look so much like a neighborhood clinic, and facility staff often told patients that their care would be covered by their health insurance, when in fact it wasn’t,” said Ho via release, who is also a professor of economics at Rice and a professor of medicine at Baylor College of Medicine.
The researchers used claims data between 2013 and 2017 from Arizona, Florida, North Carolina and Texas. Rice is part of the Blue Cross Blue Shield Alliance for Health Research, which is meant to be give health researchers access to data to better understand impactful healthcare issues. They coupled reimbursement data with counts of freestanding emergency and controlled for larger trends in emergency care in those markets.
Find the full report here.




